In November 2024, 6 months before he was to become president of the American Medical Association (AMA), Bobby Mukkamala, MD, stopped making sense. As he spoke before colleagues at an AMA meeting in Florida, the words came out all wrong.

Mukkamala, an otolaryngologist and head and neck surgeon based in Flint, Michigan, was quickly diagnosed with an 8-cm brain tumor in his left temporal lobe, a grade 2 astrocytoma. He’s been on a harrowing journey ever since, maneuvering through both a medical crisis and the troubled American healthcare system.
Just over a year after he underwent an awake craniotomy at the Mayo Clinic, Mukkamala spoke to Medscape Medical News about his experience as a patient and what it’s taught him about fixing American medicine.
“Every moment of navigating this brought to light something that we had the facts on, that I had lines in my speeches about. But to go through the system as a patient whose life depended on it was an eye-opening thing. Having this experience, not just the surgery but the aftermath, helps inform everything I say.”
When did you first realize something was wrong?
I was giving a speech to the AMA’s Minority Affairs Section at a meeting in Orlando, Florida. All of a sudden the words weren’t coming out right.
They were actual words, but they didn’t make any sense together: “I basketball play school tomorrow” instead of “I’m going to play basketball at school tomorrow.”
That had happened a few times in the prior year, and I was 53. I just thought it was me aging — a brain fart. But the people in the audience didn’t think so. Everyone thought I’d had a stroke.
My wife insisted I go to the emergency department (ED).
My vitals turned out fine, and the ED doctors thought maybe it was a transient ischemic attack. I gave a few more speeches, and everything went fine.
When did you discover what was actually happening?
When I got home [from the meeting in Florida]. A colleague of mine is a neurosurgeon, so at 9 PM I got an MRI. By 9:30 PM, I see that I have a brain tumor — a pretty big one. An 8-cm tumor in the left temporal lobe, the speech center of the brain in most people. Seizure activity within that part of my temporal lobe caused me to speak almost like babbling.
As a physician, you could read the scan yourself.
I could, though the circumstances were absurd. There are so many aspects of this that motivate me to fix what’s wrong with healthcare.
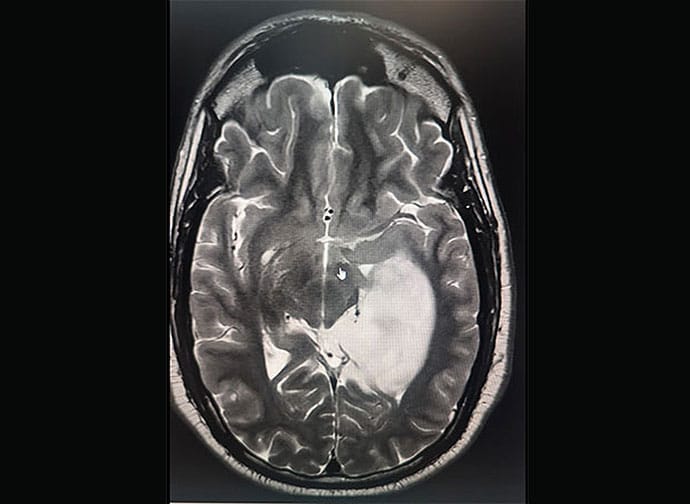
They had no blank CDs — yes, we’re still burning CDs — so there was no way to transmit the images electronically. I took out my phone, and I’m taking pictures of the monitor as the technician clicks the button to go millimeter by millimeter through my brain.
You ended up consulting six neurosurgeons in 6 days. That’s not a typical patient experience.
Not even close.
Five out of the six recommended a two-stage surgery because the tumor was so large that a full resection in one sitting risked fatal bleeding. The sixth — Dr Ian Parney at the Mayo Clinic — said he could get 90% of it out in one awake craniotomy.
Our medical knowledge — mine and my family’s — helped us evaluate those options scientifically. My mom is a retired pediatrician, my dad is a retired radiologist, and my wife is an ob/gyn.
What was it like being able to understand your situation as a physician?
Before surgery, knowing the anatomy and knowing what could go wrong was useful for making the decision about where to go and whom to trust.
Once I was in pre-op, getting the IV, and signing consent, that medical knowledge became a source of unnecessary stress. I made a conscious decision to shift into patient mode and stay there. I had faith in the team and the decision we’d made. I didn’t ask anything out of clinical curiosity because I had faith in what they were going to do.
What did this early part of your experience teach you about the healthcare system?
From the very first moment, I was realizing the failure of our healthcare system. If I had been a regular patient, I would have needed prior authorization to get an MRI scan. It would have taken a neighbor of mine in Flint weeks to get in because of a physician shortage, then a month for all the consultations. Their choice of places to go because of their insurance would be different from mine.
It was helpful to get an emotional perspective and a knowledge perspective about how the system works before I became inaugurated as AMA president. It seems goofy to say that my brain tumor was so helpful, but I just can’t help thinking about it any other way.
After your surgery, you woke up unable to speak.
The immediate, predictable thing was expressive aphasia, meaning I couldn’t talk. I remember wanting to say, “I need to go to the bathroom,” and trying to explain to people what I needed to do.
How did you manage to return to public speaking?
I did speech therapy with a therapist I’d worked with for years. She treats my patients who have speech issues from hearing loss, and now she was treating me. I pushed to speak at the AMA’s State Advocacy Summit in San Diego, just to test it. I practiced in the empty auditorium at 11 PM and 6 AM.
After speaking, I asked the AMA board what kind of grade they would give me based on how I did. They all gave me an A-plus, and I knew they were full of crap. When I forced them, they gave me a C-plus. In my mind, I’m thinking, That’s the worst grade I ever got in my life.
Weeks later, at a meeting in Washington, DC, with lawmakers, I objectively got an A-minus.
You’re taking vorasidenib, a treatment for isocitrate dehydrogenase-mutant low-grade astrocytoma or oligodendroglioma that was approved a few months before you were diagnosed. How has your experience been dealing with insurance companies?
In January, the company that sends me the medicine said something had changed about the insurance. Now, instead of a deductible of $10,000 and everything else is covered, it’s going to be about $10,000 a month — $120,000 a year.
I’m busy traveling. I spent 200 days a year on the road. I personally just don’t have time to deal with that. When they call me, I give them my wife’s number. Thank God she is willing and able to deal with them.
She’s spending time on the phone when she gets done working as an ob/gyn — her entire lunch break every day in January — trying to figure out do we really need to pay $120,000 for this?
It turns out that the prior authorization had expired. We couldn’t figure that out without me emailing the chief medical person at Blue Cross Blue Shield of Michigan that I’ve known for 25 years.
My wife didn’t want to use that privilege. I said, “Just email this guy,” so I emailed him, and within 24-48 hours, everything was approved. That is just a ridiculous healthcare system.
Were there other hassles?
They were giving me a 10-day supply of the drug, and I had a 14-day trip to Uruguay for the World Medical Association meeting. If I go a week without taking this pill, this thing could grow, and that shortens my lifespan.
Why did they give you only a 10-day supply?
If they give me 30 days, and I have a side effect and can’t take the last 20 days, it’s a waste of their money, which I kind of get. But if I need 14 days because I’m going out of the country, please put five pills at risk.
I’ve paid an insurance premium every year for 25 years. Help me? But that’s not the system we have.
How is this medicine — developed through research funded by the National Institutes of Health — affecting your prognosis?
If you Google “grade 2 astrocytoma” — which I just did last week, in case it ever changes — it says “7-10” years, something like that. And this is what it would have been. But it’s potentially very different than that because I’m on this new medicine that just got approved in August.
How might this affect your lifespan?
An early study shows that people are living longer, and I don’t think we have enough data to say how much longer. But I have everything going for me. I’m 54 now, not 64, and I’m healthy with no other comorbidities.
Your term as AMA president will end soon. What’s next for you?
I plan to be around for a decade, but I’m not planning on more than that. Likely I will be, but I want to make sure that everything that I want to do, that I need to do, that I should do, is done within a decade.
There’s one thing I’m going to do earlier than I had planned. That’s to become either a substitute teacher or a teacher of math and science in Flint public schools.
My plan is to teach math and science in the afternoon and practice otolaryngology in the morning. Flint is a small enough town that I can work in the morning at the office and the operating room, come home for lunch, and be in the classroom by 1:15. So life is good.
What do you have in mind in terms of advocacy?
I’ll use my story to talk about all of the challenges that we face and why we need to have a unified physician front. There are a million doctors in this country; we need to be unified. We want a healthier country, and we want our role as physicians to not be impeded by a system that makes that more challenging. Let’s help each other to have a healthier country.
No comments:
Post a Comment
Note: Only a member of this blog may post a comment.